In January 2020, your world got turned upside down. You were alerted by the pharmaceutically-controlled mainstream media that a frightening new “virus” had emerged from the mysterious wet food markets in Wuhan, China where the flesh of all sorts of exotic animals are sold and consumed. You were presented apocalyptic images of 4 white horsemen vans carrying the “infected” away from civilization. You were shown people dropping dead like fumagated flies in the streets. You were told that the “virus” was on its way and that it would attack your sense of taste and smell and destroy your lungs, ultimately leaving you gasping for breath and in need of invasive ventilation in order to have a fighting chance of survival. Thus, you dreaded any little symptoms that may come your way that could possibly signal that the deadly “virus” had found an entrance into your body.
In response, you locked yourself away, sanitized every chance you could get, and masked in order to protect yourself from the invisible pathogen. You avoided friends and family and made sure to keep yourself at a minimum of 6 feet away from your fellow humans who were presumed “infected” unless proven otherwise. All the while, your work life was disrupted and your financial situation was threatened. Your kids were sent home from school early and you needed a way to adjust to circumstances you were ill prepared for. Your life was thrown into a world of fear and stress unlike that which you had ever experienced before.
When the moment finally arrived and you noticed that you were experiencing some of the non-specific symptoms that the “experts” decided signaled the need to test, you quickly made your way to one of the tented testing centers the likes of which you had only witnessed in the latest zombie outbreak movie with people wrapped in ominous-looking protective gear. You had the giant Q-tip painfully shoved into your nasal passages in order to find out your fate. Sure enough, the test confirmed your worst fears as the result was positive for the terrifying “coronavirus.” It was no longer just an increasingly nagging fear in the back of your mind, it was now a fight for life and death. You accepted any treatments recommended by your doctor, whether it was antibiotics, remdesivir, supplemental oxygen, ventilation, monoclonal antibodies or some other treatment regardless of whether they were proven safe and effective.
By the saving graces of the pharmaceutical gods, you recovered from your ordeal and yet, for some reason, you were still not 100%. In fact, in some ways, your health was worse than it was before the “virus” had entered your life. You start to wonder whether you still have the dangerous entity lurking within you even though your tests were no longer positive. Worse yet, you start to question whether the “virus” did any lasting damage that you may never recuperate from. The lingering effects could not possibly have been the result of the anxiety, stress, and fear that you were subjected to leading up to and continuing on from your clash with death. It could not have possibly been due to any residual effects of the different treatments that you submitted your body to in order to fight the invisible foe. The only conclusion was that the “virus” had taken a massive toll on your body and caused chronic damage that would remain with you going forward for an indefinite period of time. You were now one of the unlucky. You were a sufferer of “long Covid.”
While the above scenario is a fictitious accounting of events, it may be a very familiar scenario for many who suffered throughout this “pandemic.” Instead of having to not only worry about catching the not-so-deadly “SARS-COV-2,” there was the potential that survival meant that the “virus” had damaged the body possibly beyond repair. Instead of overcoming “Covid” and returning to a normal state of health, one had to face the possibilty of ending up with “long Covid” and entering into a world of unpredictable chronic suffering. However, is “long Covid” a clearly definable condition or is it the mere creation of media hype and fear propaganda preying on those who were already over-stressed and in a heightened state of fear? Were the symptoms that are now associated with “long Covid” either the exacerbation of pre-existing conditions that existed prior to the “pandemic,” lingering effects from the toxic treatments used to “cure” the victims, adverse reactions to the prevantative measures involving experimental vaccination, the result of increased anxiety brought about by the fear propaganda itself, or any combination of all of the above? Let's explore the origins of the “long Covid” concept and see if we can bid it a not-so-fond farewell.
What is Regular “Covid?”
Before we can even begin to dive into what “long Covid” is, we must understand what “Covid” actually is first. It needs to be known that regular ol’ “Covid” is not actually a unique condition. There are no new or specific symptoms that define “Covid” over other respiratory diseases and ailments. When one investigates what “Covid” actually is, it is easy to see that there is no specific definition that clearly separates the disease from others. It is simply a respiratory ailment said to be caused by “SARS-COV-2.” This is how “Covid-19” is described by the WHO:
“Coronavirus disease (COVID-19) is an infectious disease caused by the SARS-CoV-2 virus.
Most people infected with the virus will experience mild to moderate respiratory illness and recover without requiring special treatment. However, some will become seriously ill and require medical attention.”
https://www.who.int/health-topics/coronavirus#tab=tab_1
According to the CDC:
“COVID-19 is a respiratory disease caused by SARS-CoV-2, a coronavirus discovered in 2019.”
https://www.cdc.gov/dotw/covid-19/index.html
The only difference between “Covid” and other respiratory ailments is the fraudulent cause associated with the exact same symptoms of disease that they all commonly share. In fact, as there are no distinct symptoms or laboratory markers separating “Covid” from other diseases, it can not be diagnosed clinically and relies upon the use of fraudulent PCR tests for diagnosis:
What about the others: differential diagnosis of COVID-19 in a German emergency department
“COVID-19 cannot be distinguished from COVID-19 negative respiratory infections by clinical signs, symptoms, or laboratory results.”
“Triage remains challenging in the emergency department since there are no reliable clinical or laboratory parameters to distinguish safely between COVID-19 and airway infections of other origins.”
https://bmcinfectdis.biomedcentral.com/articles/10.1186/s12879-021-06663-x
https://www.uptodate.com/contents/covid-19-diagnosis#H2607838323
Thus, there are no clear definitions which distinguish “Covid” from other respiratory diseases and ailments. However, like AIDS before it, the “Covid” brand did expand to include numerous unrelated conditions under its gargantuan umbrella due solely to the PCR diagnosis. In other words, if one was labelled a “Covid” case, any symptoms that they suffered from were ultimately added to the “Covid” narrative and said to be caused by “SARS-COV-2” in a game of molecular correlation equalling causation. This was despite the fact that there was no scientific evidence that a “virus” was the cause in any of these cases. This further blurred the lines as to what “Covid” actually is and it makes it impossible to really determine where regular “Covid” ends and “long Covid” begins. This lack of a clear-cut definition, however, has not stopped patient advocates from getting the equally ill-defined patient-made idea of “long Covid” into the lexicon as an accepted condition. In the absence of a formal definition, “long Covid” is used to mean any symptoms that persist after four weeks of anyone suffering from the non-specific symptoms associated with “Covid.” Interestingly, according to this letter published in September 2020, in order for “long Covid” to be clearly defined, regular “Covid” must be defined clinically outside of laboratory testing. Yet, this creates a bit of a problem as “Covid” can not be defined clinically as we discussed:
Why the Patient-Made Term 'Long Covid' is needed
What is ‘Long Covid’?
‘Long Covid’ is a patient-made term that, in the absence of formally agreed definitions, we use here to describe diverse symptoms persisting beyond four weeks after symptom onset suggestive of COVID-19. Many patients who have remained ill for months initiated support groups and grassroots campaigns to bring the condition to visibility1–3. ‘Long Covid’ (and cognate ‘long-haul Covid’) now appears in journals4,5, and has been used by clinical and governmental actors and WHO meetings6–8. Doubts and imprecision about its meaning remain, however, and an epidemiological definition is needed. For this, two other definitions must be established: a clinical case definition of COVID-19, which does not solely rely on laboratory confirmation; and a sophisticated definition for recovery that accounts for relapsing illness9,10.”
“Differential diagnosis that does not reduce ‘Long Covid’ to psychological symptoms is crucial. We urge researchers and clinicians to tread a careful line which: (i) does not assume that symptoms are caused by anxiety; (ii) acknowledges that COVID-19 is frequently a traumatic experience; (iii) considers many potential mechanisms in explaining mental health symptoms – including inflammatory responses and neurological damage21,28,35.”
https://wellcomeopenresearch.org/articles/5-224
Ironically, the above article was co-authored by the person responsible for the “Long Covid” name and concept. This ill-defined idea is a patient-made phenomenon that is heavily tied to psychological factors including anxiety brought about by trauma. “Long Covid's” roots go back to one person who tested positive by way of a fraudulent test who has a history of chronic disease. This one person was heavily influenced by the trauma that occurred when following media reports on the “novel virus” while dealing with her own issues with disease.
The Origin of “Long Covid.”
In May 2020, the hashtag #LongCovid was coined in a tweet by Dr. Elisa Perego, not a medical doctor, but rather an Honorary research member to the Institute of Archaeology at University College London. The tweet appeared to be in response to those who kept testing positive for “Covid” by PCR for at least 40 days. In her tweet, she shared an Italian article that spoke about Paul Garner, a professor of infectious diseases at the Liverpool School of Tropical Medicine, who was still positive seven weeks after the first swab. According to the professor, "The symptoms go up and down. But the coronavirus doesn't go away.” He stated that new symptoms continued to appear, one a day, "like an advent calendar.” What those symptoms were was not detailed within the article.
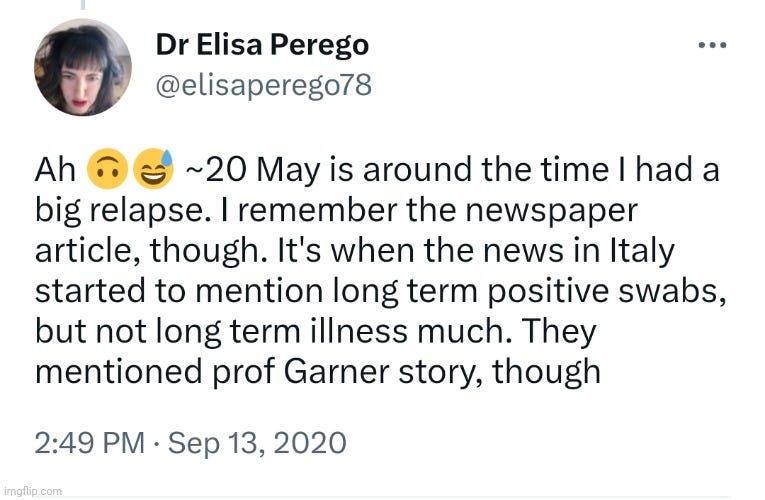
In a follow-up tweet in September 2020, Dr. Perego seemed to insinuate that, at the time, she was finding many articles on people testing positive long after “Covid” had passed but not about those who were experiencing new or lingering symptoms. It appeared that Professor Garner was the outlier.
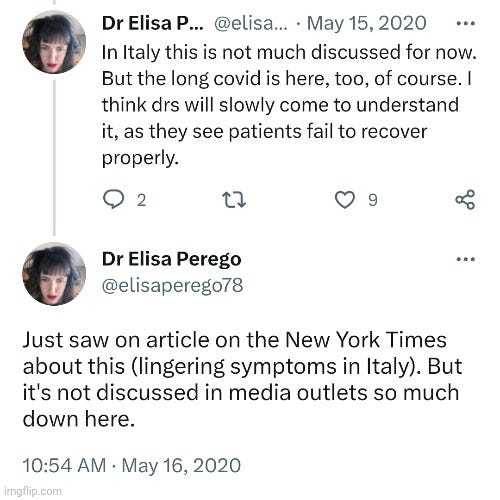
It seemed that she was referring to long-term PCR positives who did not have long-term illness with her #LongCovid hashtag rather than people who experienced lingering illness after they were no longer PCR positive. However, in tweets prior to that date, she appeared to be searching for stories of people who were still experiencing symptoms after the “virus” had passed.
Thus, Dr. Perego is given credit for coming up with the term used to identify these cases today. In fact, in an October 2022 interview, Dr. Perego, a researcher who studies health and disability in past and present societies as well as people’s responses to crises in ancient societies, discussed how she took part in a landmark WHO meeting in August 2020 where “long Covid” was recognized as a condition. This was a mere two months after coining the term, and she currently contributes to policy, research and science communication on “long Covid.”
Suffering from chronic illness since a child, Dr. Perego discussed how she was alarmed by the reports of the “novel virus” out of Wuhan. She described how she was following the story closely and felt that a storm was coming. She stated that the situation in Italy became chaotic and tragic and that, while suffering from “Covid” herself, she could not receive any care. While Dr. Perego survived her bout with “Covid,” she claimed that the disease did not go away and that, over time, new and returning symptoms began to appear which were too numerous to list. By May 2020, she suffered from what was described as a major relapse, with multi-system, cardiovascular and cardiopulmonary symptoms. Her oxygen saturation levels began to drop. This was the third month after her initial diagnosis. After seeing various reports of blood clotting in patients, Dr. Perego discussed the possibility with her primary care provider. Her “relapse” confirmed her fears that the world was dealing with a prolonged, severe, and potentially life-threatening disease that had a strong cardiovascular component. After tweeting about the prolonged positive PCR tests in May 2020, Dr. Perego's “long Covid” hashtag went “viral” and began to be used by patients and advocacy groups. According to Dr. Perego, the term became a global phenomenon:
Long COVID advocate Dr. Elisa Perego speaks on the pandemic and the need for global elimination
The World Socialist Web Site recently interviewed leading Long COVID advocate Dr. Elisa Perego, who first coined the hashtag #LongCovid in May 2020 after her experience with prolonged symptoms. Dr. Perego describes the patient-led efforts to study and educate others on Long COVID, the criminal policies implemented by numerous world governments, and the significance of historical struggles to eliminate and eradicate infectious diseases.
Evan Blake (EB): Can you tell us a bit about your background and research?
Dr. Elisa Perego (EP): I am a researcher from Italy. I also lived in the UK and Austria for study and work. As a researcher, I work across different disciplines. My background is interdisciplinary. Broadly speaking, I study social inequality, health and disability in present and past societies. My PhD is in archaeology. I was a Marie Curie Fellow at the Austrian Academy of Sciences in Vienna in 2017-19. I have also worked on human- and gene-environment interactions, climate change, and people’s responses to crises in ancient societies.
I am a person living with Long COVID and other chronic diseases since childhood. I am currently contributing to policy, research and science communication on COVID and Long COVID. I took part in the landmark WHO meeting of August 2020, which openly recognized the long-term health effects of SARS-CoV-2 infection. I tweet at @elisaperego78 about Long COVID, patient advocacy and infectious diseases in our pandemic time.
EB: What was your experience like at the start of the pandemic? My understanding is that you actually coined the hashtag #LongCovid on May 20, 2020, after your own symptoms didn’t go away. Can you share more about this? What was the response like initially and how has awareness of Long COVID developed since then?
EP: In early 2020, I was in Lombardy [Italy], the first COVID epicenter outside China. As a chronically ill person and a researcher, I was alarmed by the news about the emergence of the novel coronavirus. In January and February, I was following the growing scientific evidence closely. And then Lombardy was hit very hard. Initially, the situation was like, you know, sensing a storm that you feel is coming.
Soon, it became chaotic, tragic. Our health care system couldn’t cope with SARS-CoV-2. “Silent” community transmission wasn’t detected in time. The world saw the footage of Bergamo. I was quite ill with acute COVID, but I could not receive any meaningful medical support. I was triaged by phone, to no avail, because health care in my area was under duress.
I survived the acute pulmonary phase, but the disease progressed over time, with new symptoms and clinical signs appearing, or returning. Symptoms are too numerous to list. My cognitive impairment was severe, but I was trying to keep up with the emerging scientific data as much as I could. I was on Twitter. I could only read or write little bits at the time. I was writing privately to people about this long-term COVID illness. Long COVID is a contraction of similar terms I was using to describe my experience with COVID. This was in March and April 2020.
In May 2020, I suffered from a major relapse, with multi-system, cardiovascular and cardiopulmonary symptoms. My oxygen saturation started to drop again. I was in month three. I had the opportunity to discuss with a health care professional the possibility of clotting in my lung, which I had been concerned about. Micro-clotting and vascular damage in the lung and other body parts were being flagged as key features of severe acute COVID. But they weren’t discussed so far into the disease course.
This relapse sealed for me that we were dealing with a prolonged, severe, potentially life-threatening disease, with a strong cardiovascular component. There was also discussion, in Italy, about COVID tests that remained positive for weeks. I highlighted this in the #LongCovid hashtag tweet on 20 May 2020. Long COVID was almost immediately adopted by other COVID survivors, including creators of online support groups in the UK and many advocates. The term went viral. Professor Felicity Callard and I tell the story in “How and Why patients made Long Covid.”
I simplified the story a lot. I just want to add that I never recovered. Problems like relapsing–remitting hypoxemia, arthritis, coagulopathy and cardiovascular disease never left. Some actually became even more prominent, especially in late 2020 and early 2021. I suffered from a severe cardiopulmonary event in early 2021. I have been sharing these data across the networks of advocacy and beyond.
Cognitive impairment has improved, but I am still very affected, especially with memory loss. I am too ill to have a normal job for now. I mention my health status because I want people to know that many with Long COVID are suffering from severe disease with no appropriate support. This is despite the knowledge we already had in 2020.
Some of us have been trying to raise the alarm about the severity of the situation, in publications, in policy, but response has been slower than it should have been.
There is a lot of research available now, but we really need to translate knowledge into treatment. The costs of delays are horrendous for individuals and society alike. Lombardy has been hit by COVID wave after wave. This has greatly impacted people’s ability to obtain good medical care, including myself. More death and illness have come, too.
Italy and many other countries formally recognized Long COVID in 2020-21 and are producing guidelines. Formal recognition is important. I am happy to have contributed where I could. Long COVID is now a global phenomenon. It goes beyond medicine. It intersects with disability activism and the history of patient-led movements like HIV/AIDS. Billions are being put into new research. But access to care remains patchy. Communication of Long COVID by policymakers remains very inadequate, in my opinion. People are often unaware of the real risks of SARS-CoV-2 infection.”
https://www.wsws.org/en/articles/2022/10/10/elis-o10.html
The “long Covid” term was an ill-defined patient-made concept that was dreamt up by a chronically ill woman traumatized by the threat of the “virus” and pushed as a real phenomenon by a grassroots movement of patients. This concept was latched onto by the mainstream media hungry for frightening headlines. Even though it was accepted by the mainstream media and medical authorities as a new condition, they can not actually specifically define what “long covid” is nor show that the symptoms one is experiencing were caused by a “virus” or the disease associated with it, as admitted by the CDC:
About Long COVID
“Long COVID is a wide range of new, returning, or ongoing health problems that people experience after being infected with the virus that causes COVID-19. Most people with COVID-19 get better within a few days to a few weeks after infection, so at least four weeks after infection is the start of when Long COVID could first be identified. Anyone who was infected can experience Long COVID. Most people with Long COVID experienced symptoms days after first learning they had COVID-19, but some people who later experienced Long COVID did not know when they got infected.
There is no test that determines if your symptoms or condition is due to COVID-19. Long COVID is not one illness. Your healthcare provider considers a diagnosis of Long COVID based on your health history, including if you had a diagnosis of COVID-19 either by a positive test or by symptoms or exposure, as well as doing a health examination.”
https://www.cdc.gov/coronavirus/2019-ncov/long-term-effects/index.html
A Psychological Condition?
As stated in Dr. Perego's September 2020 letter, there is no need for a “virus” to explain “long Covid” at all. Just the threat of the “virus” is psychologically damaging enough to induce symptoms associated with “Covid,” as I pointed out in a previous article linked below. This is supported by an NIH study reported on by the Harvard Gazette in September 2022 where it was determined that psychological factors such as anxiety, depression, stress, loneliness, worry, etc. experienced before one aquired the positive “Covid” diagnosis made it much more likely for one to develop persistent symptoms associated with “long Covid.” The study followed participants from April 2020, before “long Covid” ever became a thing, and followed them for a year. They were asked questions about their psychological state throughout and, based upon when they tested positive for “Covid” and whether the symptoms lingered, it was ultimately determined that a wide range of social and psychological factors significantly increased the risk for “long Covid” and daily life impairment due to “long Covid.” Interestingly, this increased risk was independent of smoking, asthma, and other health behaviors or physical health conditions, thus placing a stronger emphasis on the role psychological distress plays in those who suffer from “long Covid.” It is well-known that a person’s mental health can exacerbate and increase the duration of symptoms experienced. The article points to both the common cold and the flu as conditions where psychological factors influence disease outcome. It is also noted that distress is associated with chronic symptoms following Lyme disease and in chronic fatigue syndrome and fibromyalgia, all of which mimic the symptoms seen in “long Covid:”
Psychological, not physical factors linked to long COVID
Psychological distress, including depression, anxiety, worry, perceived stress, and loneliness, before COVID-19 infection was associated with an increased risk of long COVID, according to researchers at Harvard T.H. Chan School of Public Health. The increased risk was independent of smoking, asthma, and other health behaviors or physical health conditions.
“We were surprised by how strongly psychological distress before a COVID-19 infection was associated with an increased risk of long COVID,” said Siwen Wang, a researcher in the Department of Nutrition at Harvard Chan School who led the study. “Distress was more strongly associated with developing long COVID than physical health risk factors such as obesity, asthma, and hypertension.”
“Mental health is known to affect the outcomes of some diseases. Depression and other mental illnesses have been associated with greater risk of more severe COVID-19 including the risk of hospitalization, which is a risk factor for long COVID. In other acute respiratory tract infections, such as flu or common cold, mental health conditions are associated with greater severity and longer duration of symptoms. Previous studies have also suggested that distress is associated with chronic symptoms following Lyme disease and in chronic fatigue syndrome and fibromyalgia, which have symptoms similar to those of long COVID.
To determine the effects of psychological distress before COVID-19 infection on developing long COVID, Wang and her colleagues enrolled more than 54,000 people in April 2020. At the beginning of the study, the researchers asked the participants about their psychological distress. Over the following year, more than 3,000 participants contracted COVID-19, and the researchers asked participants about their COVID-19 symptoms and symptom duration.
After analyzing the responses and comparing those who developed long COVID to those who did not, the researchers determined that distress before COVID-19 infection, including depression, anxiety, worry, perceived stress, and loneliness, was associated with a 32 percent to 46 percent increased risk of long COVID. These types of psychological distress were also associated with 15 percent to 51 percent greater risk of daily life impairment due to long COVID.
“To the best of our knowledge, this is the first prospective study to show that a wide range of social and psychological factors are risk factors for long COVID and daily life impairment due to long COVID,” said Andrea Roberts, senior research scientist in the Department of Environmental Health at Harvard Chan School and senior author of the JAMA Psychiatry paper. “We need to consider psychological health in addition to physical health as risk factors of long COVID-19. These results also reinforce the need to increase public awareness of the importance of mental health and to get mental health care for people who need it, including increasing the supply of mental health clinicians and improving access to care.”
Dr. Perego seemed to be in a heightened state of distress judging by her recounting of events leading up to the “long Covid” hashtag. She was reading stories about the “novel virus” and worried about the chaos and tragedy she was seeing in the media. Could her “long Covid” symptoms have been brought about by her psychological state leading up to and after her diagnosis as suggested by the study referenced above? Could this distress have exacerbated her chronic illness that she was suffering from since childhood? What medications was she taking leading up to, during, and after her diagnosis? Could these have also contributed to her health status? Judging by the next two cases, the care one receives can also play a role in bringing about the symptoms associated with “long Covid:”
A Pharmaceutical Condition?
People often forget that the medications and the treatments that they receive upon visit to the doctor and/or the ER can be potentially more damaging than the initial symptoms that they presented with. Pharmaceuticals come with various side-effects that not only mimic the diseases that they are used to treat, but can also lead to a worsening condition. Steroids used to treat inflammation come with a laundry list of dangerous adverse reactions. Medical interventions such as invasive ventilation can damage the lungs irrepably by inducing a condition known as ventilator-induced lung injury (VILI). These treatments alone could leave someone in a much worse state after the “virus” has been said to have passed that can take months to years for the patient to recover from.
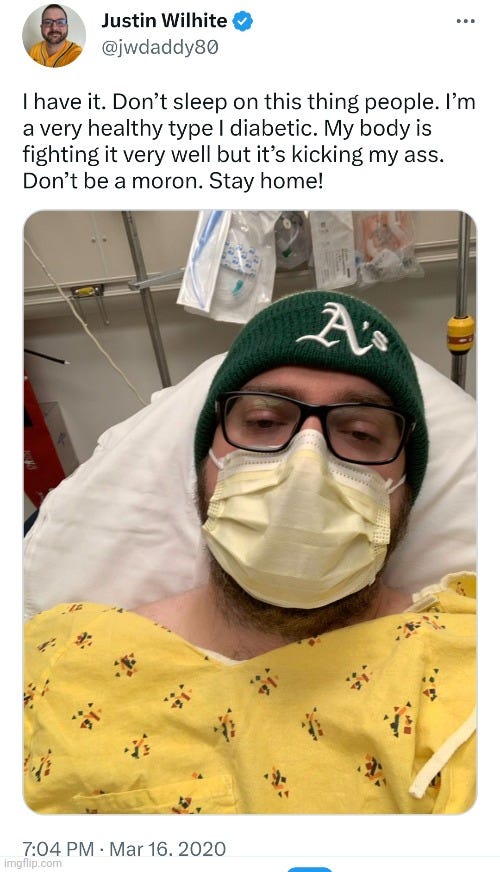
For example, Justin Wilhite is a Rancho Cordova man who was said to have caught “SARS-COV-2” back in March 2020. Wilhite was featured in multiple stories by ABC10, with the first one published on March 17th, 2020 discussing his battle with the disease. In the initial report, it was stated that Wilhite was certain that he was fighting the “coronavirus” despite no positive test confirming his belief (i.e. fear) at the time. It was mentioned that he is a Type 1 diabetic, thus he had an already established pre-existing health condition like many “Covid” patients. While claiming that he is very healthy, Wilhite said that the “virus” had taken quite a toll on him, even though he chalked his initial symptoms up to allergies. The article mentioned that Wilhite passed out, which resulted in his seeking treatment at the hospital where he was diagnosed with and treated for the flu. Wilhite was never tested for “SARS-COV-2” due to a lack of tests and it was later assumed by his doctor that he had the “coronavirus:”
'This isn't the flu' | Rancho Cordova man's Twitter thread urges people to take coronavirus seriously
“A Rancho Cordova man has taken to Twitter, warning people to take the coronavirus pandemic more seriously. Even though he wasn't given a test at the hospital, Jusin Wilhite believes he has coronavirus.
“Don’t sleep on this thing people,” Wilhite wrote on social media.
Wilhite, a 39 year-old Type I diabetic from Rancho Cordova, is currently quarantined with his family. Though he describes himself as “very healthy,” he writes the coronavirus has taken quite a toll on his health.
Feeding his followers’ curiosity, Wilhite details the progression of his symptoms in a Twitter thread. He says his symptoms started as early as two weeks ago.
“March 4th I began getting a headache and I could feel my lungs, which is weird,” Wilhite writes. “But everything is blooming so I chalked it up to allergies. My breathing became progressively more labored and began to hurt.”
“Wilhite continued his Twitter thread noting he went to the Emergency Room after passing out and having difficulty breathing, but medical staff treated him for the flu, unaware that he was carrying coronavirus. However, he was simply not recovering, despite flu medication that doctors gave him and soon returned to the ER.
Wilhite did not get a coronavirus test administered. He told ABC10, doctors told him and his wife there is a lack of resources when it comes to the tests. He said his doctor believes he has the coronavirus.”
In a series of tweets recounting his ordeal, Wilhite described how, unlike the reporting by ABC10, he nearly passed out which led him to go to the ER. The treatments that he received while at the hospital and at home, such as Tamiflu, Motrin, an inhaler, and the steroid prednisone, actually made his condition worse:
On July 29th, 2020, ABC10 did a follow-up on Wilhite where he claimed to be suffering from lung damage, brain fog, and upper respiratory issues after his bout with “Covid.” It was stated that he was in and out of the hospital for treatments at the time. While this second article said that he eventually tested positive for “SARS-COV-2,” no date was given as to when this occurred:
Rancho Cordova man who beat coronavirus helps create coalition for other survivors
“A Rancho Cordova man who survived the coronavirus is now aiming to help others like him by forming a coalition of survivors.
Justin Wilhite said the long-term effects of the virus are difficult and many symptoms still linger.
"I'm kind of sick of being sick at this point and it's been a long time since I've been healthy," Wilhite said.
Wilhite, 39, survived the coronavirus. ABC10 spoke with him in March when he was at his worst.
Wilhite said he had a hard time getting a test at first and was in and out of the hospital. Eventually, he said he tested positive and recovered at home. But still, nearly five months later, he isn't 100 percent.
"I truly didn't expect for this to last as long," Wilhite said.
He has lung damage, he can't walk long distances without getting winded, he has severe brain fog and upper respiratory issues.”
On March 6th, 2023, ABC10 followed up with Justin Wilhite for an update three years after his ordeal. It was stated that he has been suffering “long Covid” ever since the time that he thought he caught the “virus” at work and came down with symptoms on March 4th, 2020. He described his initial difficulty breathing as feeling like there was glass in his lungs, a description that was most likely propagated by the numerous reports of the non-specific CT findings of ground-glass opacities in the lungs of some victims. Justin stated that every day he deals with incredible fatigue and shortness of breath since his initial symptoms presented themselves on March 4th.
Interestingly, according to Dr. Brad Sanville, who was interviewed for the article, those experiencing fatigue and shortness of breath don't always have lung and heart damage. He chalked their symptoms up to chronic fatigue syndrome, something that existed “pre-Covid” with reports of similar cases going as far back as 1750. He stated that these people are mistaking symptoms of fatigue with the feeling of shortness of breath. Of course, the doctor said that studies suggested that those who are vaccinated are less likely to develop “long Covid” as the toxic agenda must be pushed with every chance they get. However, Dr. Sanville also stated that the majority of the “long Covid” cases never required hospitalization. These are people with “stay-at-home” symptoms that have something drastic change in their lives before experiencing “long Covid,” thus alluding to the fact that there is more to this story, such as the psychological trauma discussed earlier, than a fictional “virus:”
‘It's been this way every day since March 4, 2020’ | Long COVID patient shares story of suffering
“42-year-old Justin Wilhite lives with his wife and three sons in Rancho Cordova. He has been suffering from the effects of post acute COVID syndrome – commonly known as “long COVID” – for three years now.
“I'm just a person that got COVID in the first wave, March 2020…I'm just living with the post effects of that,” he said. “March 4, (2020), I wake up, I have a headache. My lungs kind of feel like glass. I feel really short of breath.”
Wilhite has Type 1 Diabetes, one of the health conditions that puts someone at greater risk of getting a serious COVID infection. He thinks he caught the virus at work—and the effects are still lingering.
“Every day I deal with incredible fatigue, shortness of breath -- and that's just getting up, walking to the bathroom,” Wilhite said. “My daily activity -- and it wipes me out and it acts like a workout for me - is going downstairs and back up. If I do that three times, the next day, my legs don't work….and it's been this way, every day, since March 4, 2020.”
“Long COVID patients with shortness of breath or trouble walking don’t always have lung or heart damage, he said. Rather, chronic fatigue syndrome could be to blame.
“The fatigue, I think, is so overpowering for people, it makes them perceive everything as being short of breath, when – really - it might just be really profound fatigue. And we can't find anything, like, obviously wrong with their lungs or their heart to explain it,” Dr. Sanville said.”
“As for Dr. Sanville, he said there’s some research that suggests a person is less likely to have long COVID symptoms if they’re vaccinated, so he encourages people to keep up on vaccinations and boosters to protect themselves.
Most people he sees with long COVID had a case that did not require hospitalization.
“Most of the people we see are people that had stay-at-home symptoms and - for whatever reason - have had a drastic change in something in their life. And why that is the case, I don't think is really fully understood quite yet,” he said. “It's a little concerning that you could just get it and have it seem like a cold and then have life-changing symptoms for a long time.”
When one looks at the treatments Wilhite endured, both Tamiflu and prednisone alone can result in the same symptoms that Wilhite suffers from such as brain fog, anxiety, and difficulty breathing. It is entirely possible that the treatments, along with the psychological trauma he experienced, led to Wilhite's worsening state and continued symptoms presenting as “long Covid.” However, the treatments themselves are rarely investigated as potential causes and/or contributing factors. When they are loosely investigated, such as in the case of the “Covid” vaccines, there is evidence to suggest that these treatments are directly related to the continued problems that the patients are suffering from.
This was seen in the case of Brianne Dressen, a clinical trial volunteer for the AstraZeneca vaccine, who was never diagnosed with “Covid-19.” After her first dose of the vaccine, she started experiencing symptoms that eventually mimicked what others were experiencing with “long Covid.” While her doctor diagnosed her with anxiety, she and her husband continued to investigate and found others suffering similar problems after vaccination, regardless of the vaccine given. This eventually lead to the NIH bringing Dressen and others in to study this phenomenon. While the NIH efforts ultimately stalled and the data was never reported, a small number of other researchers worldwide are now studying the “biology of long Covid,” which is still considered to be poorly understood, and the association with postvaccine side effects. However, even then, top medical journals are declining to publish any results as they are considered observational, even though the vast majority of the evidence for “SARS-COV-2” is epidemiological, which are observational studies. While vaccinemakers like Pfizer understand that there is a problem and are said to be investigating this connection, scientists and researchers are afraid to touch the issue. Thus, the link between the toxic vaccines and the longterm damage mimicking “long Covid” is vastly understudied:
In rare cases, coronavirus vaccines may cause Long Covid–like symptoms
Brain fog, headaches, blood pressure swings are being probed by NIH and other researchers
“In late 2020, Brianne Dressen began to spend hours in online communities for people with Long Covid, a chronic, disabling syndrome that can follow a bout with the virus. “For months, I just lurked there,” says Dressen, a former preschool teacher in Saratoga Springs, Utah, “reviewing post after post of symptoms that were just like my own.”
Dressen had never had COVID-19. But that November, she’d received a dose of AstraZeneca’s vaccine as a volunteer in a clinical trial. By that evening, her vision blurred and sound became distorted—“I felt like I had two seashells on my ears,” she says. Her symptoms rapidly worsened and multiplied, ultimately including heart rate fluctuations, severe muscle weakness, and what she describes as debilitating internal electric shocks.
A doctor diagnosed her with anxiety. Her husband, Brian Dressen, a chemist, began to comb the scientific literature, desperate to help his wife, a former rock climber who now spent most of her time in a darkened room, unable to brush her teeth or tolerate her young children’s touch.
As time passed, the Dressens found other people who had experienced serious, long-lasting health problems after a COVID-19 vaccine, regardless of the manufacturer. By January 2021, researchers at the National Institutes of Health (NIH) began to hear about such reports and sought to learn more, bringing Brianne Dressen and other affected people to the agency’s headquarters for testing and sometimes treatment.”
“NIH’s communications with patients faded by late 2021, though Nath says the work continues behind the scenes. The pullback caused bewilderment and dismay among patients who spoke with Science, who said the NIH researchers were the only ones helping them. Now, a small number of other researchers worldwide is beginning to study whether the biology of Long Covid, itself still poorly understood, overlaps with the mysterious mechanisms driving certain postvaccine side effects.”
Echoes of Long Covid?
“How frequently side effects like Dressen’s occur is unclear. Online communities can include many thousands of participants, but no one is publicly tracking these cases, which are variable and difficult to diagnose or even categorize. The symptoms also include fatigue, severe headaches, nerve pain, blood pressure swings, and short-term memory problems. Nath is convinced they are “extremely rare.”
“The NIH data, which documented the patient cases, haven’t been reported yet. Two top medical journals declined to publish a case series of about 30 people, which Nath first submitted in March 2021. Nath says he understands the rejection. The data weren’t “cut and dried; it was observational studies.” This month, the scientists submitted a case series of 23 people to a third publication, and Nath says his group has submitted an amendment to a Long Covid protocol to include patients with postvaccine side effects.”
“Science contacted regulators and vaccinemakers about any information they’d gleaned on these side effects. A Pfizer spokesperson wrote, “We can confirm it’s something we’re monitoring.” Moderna, AstraZeneca, and Johnson & Johnson all said they take side effects seriously and share reports they receive with regulators. An FDA spokesperson said the agency “continues to maintain a strong focus on monitoring the safety of the COVID-19 vaccines,” while the European Medicines Agency notes it “is taking steps to use real-world data from clinical practice to monitor the safety and effectiveness of COVID-19 treatments and vaccines.”
Other researchers note the scientific community is uneasy about studying such effects. “Everyone is tiptoeing around it,” Pretorius says. “I’ve talked to a lot of clinicians and researchers at various universities, and they don’t want to touch it.”
“Cheng has heard from dozens of people who describe chronic postvaccine problems, and she finds the overlap between their symptoms and those of Long Covid compelling. Now, she wants to move deliberately and scientifically in a search for answers. “We’ve got to retain rigor,” she says. “There’s just this complete dearth of data.”
A Media-Hyped Patient-Made Condition
According to the WHO, there are now more than 200 symptoms associated with the ill-defined hashtag-driven phenomenon known as “long Covid.” In other words, every possible symptom one experienced after a positive PCR test was lumped together with all others under a nifthy little label whether related or not. However, as is the case with “regular Covid,” there is no scientific evidence proving that any of these symptoms associated with “long Covid” were ever the result of any “novel virus.” When studies have investigated other potential contributing factors, there has been a clear association between the psychological trauma one experiences before the fraudulent diagnosis as well as evidence that the experimental injections could be having an effect as well. Whether future research will further investigate the role that psychological distress and toxic treatments, alone and in combination, play into a worsening chronic health status remains to be seen. Judging by the past, these findings will be brushed aside in favor of generating pseudoscientific fantasy detailing how the invisible “virus” invades certain organs and neurological pathways in order to bring about this cascading series of non-specific symptoms in order to push the injections as the savior, just as Dr. Sanville suggested.
And therein lies the problem. When the focus is on the invisible boogeyman, all attention and financial resources are put towards creating stories to hypothetically explain how this fictional entity can do so much damage. Meanwhile, real factors such as the psychological trauma and pharmaceutical poisons become an afterthought. The “virus” becomes a convenient way to keep people focused on looking one way while ensuring that their eyes do not wander anywhere else. The threat of the patient-made media-driven long-lasting effects of “long Covid” has become a useful tool to keep people frightened of the non-existent pathogen in order to ensure that their sleeves remain rolled up for the experimental vaccines and subsequent boosters. The non-specific and ill-defined nature of “long Covid” lends itself perfectly as a way to cover up any potential toxic fallout induced by this fear propaganda-driven “pandemic.” It wasn't the stress and trauma generated by 24/7 media fear porn. It wasn’t the dangerous pharmaceuticals and invasive ventilation used haphazardly as a treatment. It wasn't the toxic experimental vaccine given as a preventative measure. It was the little ol’ “virus” that did all of this devastating damage. Virologists, scientists, clinicians, and researchers can't define “long Covid” and they have no idea as to how the “virus” manages such a feat as to create long-lasting chronic health effects, but rest assured, they will keep chasing ghosts until they find out.
Here are two related articles that help to add further context to concepts brought up within this article:
Differential Diagnosis?
differential diagnosis : the distinguishing of a disease or condition from others presenting with similar signs and symptoms https://www.merriam-webster.com/dictionary/differential%20diagnosis I imagine most of us have “fond” memories of going to the doctor when feeling unwell and getting subsequently poked and prodded in order to determine a “cause” for t…
Fear is the Real "Virus"
There is an invisible pathogen out there infecting the population. It is a contagion as old as time itself and it is one that is powerful enough to disrupt society, bringing down the strongest of civilizations. It can infect anyone at any time and if we are not careful, we can easily pass this unseen entity onto those around us. Worse yet, we can pass it on to our children, setting them up with a chronic lifetime infection that may never be cured, spreading from generation to future generation. What I am discussing here is not the typical perception of the pathogenic “virus” floating about infecting us and causing disease as these entities have never been scientifically proven to exist. However, there is one thing that truly does exist which fits the concept of a “virus” far better than any obligate intracellular parasite ever could. I am talking about the one true “virus:” the “virus” called fear.



















A few other things I might highlight in bold in that ridiculous interview this “Dr.” Perego (who looks like she resides on the streets of SF) gives with the "World Socialist" website (itself a major clue as to the deceptive types we’re dealing with here). Like all the other con-artists who are front and center in this scam, she plays the Hegelian dialectic by assuming “facts” that are unconfirmed (always begging the question about the assumed "problem") and, as her primary MO, uses emotional fear-based language to get you to "react," while then moving on to what "we" (the collective) must do to deal with the situation (offering "solutions"). Her regular very loose use of emotional and hyperbolic language is illustrative as anything of the (real) "fact" that the whole thing is propaganda warfare and a scam.
Examples from the interview:
-- she says she studies “climate change” (always assumed to an actual phenomenon)
-- references “our pandemic time” (we're in an era of “pandemics”)
-- uses dramatic, run-for-the-hills-type language over and over again: “Lombardy was hit very hard…Soon, it became chaotic, tragic”; “Our health care system couldn’t cope…health care in my area was under duress” (the region got "hit" "very hard” and it soon became “chaotic,” “tragic," where “the virus” was so out of control, our systems couldn't cope; there was nothing we could do!)
-- more of the same fear-inducing language when she says we must “raise the alarm about the severity of the situation”; “Lombardy has been hit by COVID wave after wave,” and “more death and illness have come, too” ("alarm," "severity," "hit," "wave after wave," "death" and "illness")
-- states that “symptoms are too numerous to list” (the “virus” is so deadly, it produces innumerable unnamed symptoms!)
-- says that “COVID tests remained positive for weeks” (don’t know what to make of this, as this is illogical. How does a test “remain” positive? A test has no “duration”; a test indicates something momentarily. What is she talking about?)
-- on the personal front, says that she is “too ill to have a normal job for now…I never recovered” (she herself got hit and the thing is so deadly, she lost her “normal” life and “never recovered" and thus, by implication, SO COULD YOU)
-- references the collective "we" and the horror the situation ("problem") poses. Accordingly, "we" require that a "treatment" ("solution") be implemented and deployed: “the costs of delays are horrendous for individuals and society alike” and “we really need to translate knowledge into treatment”
Over and over in that interview, she uses classic propagandizing, fear-inducing language to excite you to a reaction. Something MUST be immediately done to try to treat "it" (the thing assumed to exist and wreaking death and destruction across the land). And we cannot delay in dealing with it, as the results WILL be (“are”) “horrendous.” We must proceed to the treatment stage (the “solution”).
Ugh.
I find the stories of those with multiple issues before cv19 blaming their issues on COVID as disingenuous.
Perhaps they were convinced that their condition got worse due to the disease, but honestly, how do we know they weren't damaged by remdesevir or the other drugs like tamiflu?
Also, why would having oxygen below 85% justify a ventilator? That's asking for trouble and before COVID was never the process. Ventilators are for those that cannot breathe in the first place... Not to help people breathe. Supplying oxygen is the norm but it seems that COVID made a lot of the medical system turn into an Idiocracy.
Whatever, this whole thing just helps people realize that medicine is far from scientific. It's very much politically and economically motivated.
The more people realize this, the better.