Over the last few seasons of this lovely little game of “pandemics” we’ve found ourselves in, every fall leading into winter there have been whispers and murmurs about the coming of the “Twindemic.”
We have been warned of the potential threat of facing not only the dreaded army of “SARS-COV-2” and its variants-of-concern but also the re-emergence of the forgotten bastard son known as influenza and its mutant army. Together, they will attack the population, with “Covid” targeting the unvaccinated while the flu cleans up the vaccinated who somehow ignorantly destroyed their own prior influenza defenses by wearing a mask.
“When people began isolating, social distancing and masking to slow the spread of Covid-19 in early 2020, flu all but disappeared in the US. As a result, most people haven't been exposed to influenza for a few years, meaning immunity against flu viruses could be low and underscoring the need to get vaccinated.”
https://www.google.com/amp/s/amp.cnn.com/cnn/2022/10/14/health/flu-season-concern/index.html
The delicious irony is that the very measures used to “protect” us from “Covid” and scattered the flu back into oblivion are now coming back to haunt us. This is supposedly happening in the form of decreased immunity due to a lack of exposure to the absent influenza. The creative visionaries of the vaccine propaganda couldn't have written a better plot-line to push their products onto the frightened populace.
So here we are entering our third year of the looming threat of the Twindemic. It has been heavily promoted the last few seasons. Is it finally time for the battle of the century? According to the showrunners, it sure appears that way. This year, we apparently know for certain that the flu is back in a big way due to the severity of the flu season in Australia foreshadowing what will happen elsewhere. Spoilers! Thus, the predictions are for a rerun of the flu seasons of years past to coincide with the brand new “Covid” variant spin-off. These two “viruses” will partake in an epic battle to secure the throne and claim the rightful title of the baddest pathogen in Westeros…ahem, I mean, on Earth:
Is the flu making a comeback after a COVID-19 pandemic lull?
“After skipping two seasons in the Southern Hemisphere, flu spent 2022 hopping across the planet’s lower half with more fervor than it’s had since the COVID crisis began. And of the three years of the pandemic that have played out so far, this one is previewing the strongest signs yet of a rough flu season ahead,” Wu writes.
Flu was pretty much absent during the first winter of the COVID-19 pandemic as people masked up and took other precautions to prevent its spread, steps that also helped stop influenza in its tracks. Last year, some flu cases emerged and lingered into the spring, but a severe outbreak never came.
This year might be very different north of the equator.
“It’s been a really, really bad influenza season down in Australia. We have potential for a pretty bad (season),” Dr. Tamara Sheffield, medical director of preventative medicine for Intermountain Healthcare, said recently, stressing the need for Utahns to start planning for their annual flu shot.”
“When omicron cases started dropping, the doctor said, “all of a sudden, we had influenza pop up again that next month,” before another strain of omicron surfaced. Flu and COVID-19 “kind of compete with each other, of who’s going to make you sick,” she said.”
Of course, it wouldn't be a satisfying battle without the entry of a new weapon to save the day. Fortunately, the writers have just what we need as the armies of Pfizer to the South as well as those of Moderna to the North are bringing their experimental mRNA technology with them in order to combat both “viruses” this season. So if the threat of the Twindemic has you on the edge of your seat, fear not as the pharmaceutical gods have heard your prayers and have conjured up another round of injections which are headed your way in order to boost you through the potential catastrophic event 3 years in the making:
It's flu vaccine time and seniors need revved-up shots
“While there’s no way to predict if the U.S. will be as hard-hit, “last year we were going into flu season not knowing if flu was around or not. This year we know flu is back,” said influenza specialist Richard Webby of St. Jude Children’s Research Hospital in Memphis.”
“Australia just experienced its worst flu season in five years and what happens in Southern Hemisphere winters often foreshadows what Northern countries can expect, said Dr. Andrew Pekosz of the Johns Hopkins Bloomberg School of Public Health.
And people have largely abandoned masking and distancing precautions that earlier in the pandemic also helped prevent the spread of other respiratory bugs like the flu.”
“This poses a risk especially to young children who may not have had much if any previous exposure to influenza viruses prior to this season,” Pekosz added.
“This year we will have a true influenza season like we saw before the pandemic,” said Dr. Jason Newland, a pediatric infectious disease specialist at Washington University in St. Louis.”
FLU SHOTS OF THE FUTURE
“The companies that make the two most widely used COVID-19 vaccines now are testing flu shots made with the same technology. One reason: When influenza mutates, the recipes of so-called mRNA vaccines could be updated more quickly than today’s flu shots, most of which are made by growing influenza virus in chicken eggs.
Pfizer and its partner BioNTech are recruiting 25,000 healthy U.S. adults to receive either its experimental influenza shot or a regular kind, to see how effective the new approach proves this flu season.”
https://www.yahoo.com/lifestyle/flu-vaccine-time-seniors-revved-051111857.html
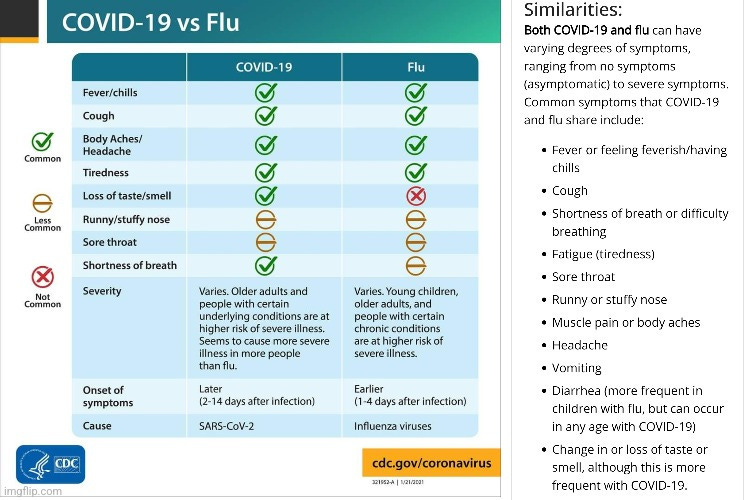
If this critic is being honest, it really feels like we just being sold the same old recycled plotline year in and year out at this point. Is there really any differences between the two villains vying for the throne or are they the same actor with a hip new name and a wardrobe change? Let's review some of the storylines of the past and see what we can find out. According to the CDC, influenza and “Covid-19” are, for all intents and purposes, identical:
“You cannot tell the difference between flu and COVID-19 by the symptoms alone because they have some of the same signs and symptoms. Specific testing is needed to tell what the illness is and to confirm a diagnosis. Having a medical professional administer a specific test that detects both flu and COVID-19 allows you to get diagnosed and treated for the specific virus you have more quickly.”
https://www.cdc.gov/flu/symptoms/flu-vs-covid19.htm
As the two “viruses” present with the exact same symptoms of disease, it is impossible to differentiate them by way of clinical diagnosis based solely on the symptoms. What this means is that the only possible way to diagnose someone with either “virus” is through the use of “diagnostic” tests. However, this creates some huge plot holes which sadly the writers failed to address. First off, as neither “virus” has ever been properly purified and isolated from the fluids of a sick host, the tests have never been calibrated and validated against the gold standard of actual “viral” particles. Thus, as no “viruses” were used in the creation of the tests, these tests are unable to detect either one in order to distinguish between the two.
However, even if the tests had been properly calibrated and validated to actual “virus,” both PCR and rapid antigen tests require disease prevalence to be known in order for the results to be considered accurate. As defined by the CDC, prevalence is “the proportion of persons in a population who have a particular disease or attribute at a specified point in time or over a specified period of time.” This is how the CDC calculates disease prevalence:
In order to determine prevalence, cases must be known and must come from diagnosis based on clinical symptoms alone. However, as the symptoms are identical between influenza, “Covid-19,” and many other diseases, there is no way to diagnose a patient clinically in order to differentiate cases and thus there is no way to determine disease prevalence. Without knowing diseaee prevalence, there is no way to determine whether or not any of the test results are being interpreted accurately. In order to get around this unfortunate roadblock, researchers use the PCR test to create the cases used to determine disease prevalence in order to say that the PCR results are accurate based upon the PCR-manufactured prevalence rate. This is an entirely fraudulent process as PCR can not be used to generate cases in order to claim its own results are accurate. The writers have developed an insane circular trap that they have yet to credibly explain.
Regardless of these glaring plot holes, the medical institutions will provide contradictory statements that make matters even more confusing. For example, the writers at the WHO state that the majority of flu cases are diagnosed clinically. However, within the same paragraph they contradict themselves by admitting that other respiratory “viruses” make clinical diagnosis difficult (i.e. impossible) as they present with the same exact symptoms. Adding further confirmation that their original clinical diagnosis claim was false, the writers state that a definitive diagnosis of influenza can only come by the application of a laboratory diagnostic testing. The writers point out that Rapid influenza diagnostic tests (RIDTs) are used in clinical settings, yet these tests have a lower sensitivity compared to RT-PCR methods and are considered less “accurate.” Thus, the reliability of the RIDT's largely depends upon the conditions under which they are used. As we already covered, without the ability to diagnose a disease clinically in order to get an accurate disease prevalence rate, none of the tests can provide an “accurate definitive diagnosis:”
Diagnosis
“The majority of cases of human influenza are clinically diagnosed. However, during periods of low influenza activity and outside of epidemics situations, the infection of other respiratory viruses e.g. rhinovirus, respiratory syncytial virus, parainfluenza and adenovirus can also present as Influenza-like Illness (ILI) which makes the clinical differentiation of influenza from other pathogens difficult.
Collection of appropriate respiratory samples and the application of a laboratory diagnostic test is required to establish a definitive diagnosis. Proper collection, storage and transport of respiratory specimens is the essential first step for laboratory detection of influenza virus infections. Laboratory confirmation of influenza virus from throat, nasal and nasopharyngeal secretions or tracheal aspirate or washings is commonly performed using direct antigen detection, virus isolation, or detection of influenza-specific RNA by reverse transcriptase-polymerase chain reaction (RT-PCR). Various guidance on the laboratory techniques is published and updated by WHO. (3)
Rapid influenza diagnostic tests (RIDTs) are used in clinical settings, but they have lower sensitivity compared to RT-PCR methods and their reliability depends largely on the conditions under which they are used.”
https://www.who.int/news-room/fact-sheets/detail/influenza-(seasonal)
As we saw earlier from the writers at the CDC, they contradict the wish-washy clinical diagnosis claim made by the WHO by stating defiantly that influenza and “Covid-19” (as well as other respiratory “viruses”) can not be diagnosed clinically. The only way to figure out which patient has which “virus” is through laboratory testing. However even then, in the case of the flu, clinicians may choose not to do a test on someone suspected to have influenza. In other words, it can be assumed that the patient has influenza and not some other “virus” whenever the doctor decides that “definitive laboratory testing” is not required. Fortunately there is agreement between the writers at the WHO and the CDC as they both call into question the accuracy of the RIDT's used to diagnose influenza as it is hindered by false-negative and false-positive results based upon the disease prevalence given at the time. Please note that this is the same disease prevalence rate that requires the ability to diagnosis cases clinically in order to determine an accurate rate…which is considered impossible for respiratory “viruses.” See the problem yet?
“A number of tests can help in the diagnosis of influenza (see table). But, tests do not need to be done on all patients with suspected influenza. For individual patients, tests are most useful when they are likely to yield clinically useful results that will help with diagnosis and treatment decisions.”
“Because of the lower sensitivity of the rapid influenza diagnostic tests, physicians should consider confirming negative test results with RT-PCR, viral culture or other means, especially in hospitalized patients or during suspected institutional influenza outbreaks because of the possibility of false-negative RIDT results, especially during periods of peak community influenza activity. In contrast, false-positive RIDT results are less likely, but can occur during periods of low influenza activity. Therefore, when interpreting results of a rapid influenza diagnostic test, physicians should consider the positive and negative predictive values of the test in the context of the level of influenza activity in their community. Package inserts and the laboratory performing the test should be consulted for more details regarding use of rapid influenza diagnostic tests.”
https://www.cdc.gov/flu/professionals/diagnosis/labrolesprocedures.htm

Despite this prevalence problem, the CDC's protocol for diagnosing influenza and/or “SARS-COV-2” is based solely on the fraudulent tests. However, the writers make an important caveat to only test for influenza if the results will change clinical management or for infection control decisions. In fact, antivral treatments can be prescribed based solely upon empirical evidence as soon as possible without influenza testing based upon a clinical diagnosis of influenza for patients of any age with progressive disease of any duration. Thus, the CDC allows for the use of clinical diagnosis to determine an influenza case for treatment even though it said this was impossible to determine clinically without testing. In other words, “SARS-COV-2” testing is required for “definitive diagnosis” but influenza testing can be skipped based on a negative “SARS-COV-2” result and the determination that there is no benefit to testing. This in turn allows for influenza cases to be assumed and treatment to be given without any “definitive diagnosis:”
Follow recommended infection prevention and control measures
SARS-CoV-2 TestingTest for SARS-CoV-2 by nucleic acid detection2,3; OR if not available, by SARS-CoV-2 antigen detection assay.5
a) If SARS-CoV-2 Test result is positive, administer supportive care. If the patient is at high risk for progression to severe COVID-19, prescribe treatment for nonhospitalized patients as recommended per NIH COVID-19 Treatment Guidelines.7
For adult patients with suspected community-acquired pneumonia who do not require admission, see American Thoracic Society-Infectious Diseases Society of America Adult Community-acquired Pneumonia Guidelines6
For otherwise healthy non-high-risk persons with influenza-like illness (fever and either cough or sore throat) with illness ≤2 days, empiric antiviral treatment can be prescribed based upon clinical judgement.11,12
For otherwise healthy non-high-risk persons without influenza-like illness or with illness duration >2 days, antiviral treatment of influenza is unlikely to provide significant clinical benefit.11
Influenza Testing and Treatment
a) Test for influenza if results will change clinical management or for infection control decisions (e.g. long-term care facility resident returning to a facility, or a person of any age returning to a congregate setting): order rapid influenza nucleic acid detection assay2,3,4,11; if rapid influenza nucleic acid detection assay is not available on-site, order rapid influenza antigen assay13; prescribe antiviral treatment if positive.11,12ORb) Prescribe empiric antiviral treatment as soon as possible without influenza testing based on a clinical diagnosis of influenza for patients of any age with progressive disease of any duration, and for children and adults at high risk for influenza complications.11,12,14Follow isolation and quarantine recommendations for SARS-CoV-2
https://www.cdc.gov/flu/professionals/diagnosis/testing-guidance-for-clinicians.htm
Interestingly, the writers admit that even with these measures, “SARS-COV-2” isolation and quarantine recommendations should be followed regardless of whether one is considered positive for “SARS-COV-2” or influenza. Why would they recommend the same actions for different “viruses?” Perhaps this is because the only difference between the two “viruses,” as stated by the WHO, are the treatments which are given. Or perhaps this is because the diagnosis is utterly meaningless as it is said by the CDC that positive results for one “virus” does not exclude the patient from having the other:
(Note: Because SARS-CoV-2 and influenza virus co-infection can occur, a positive influenza test result without SARS-CoV-2 testing does not exclude COVID-19, and a positive SARS-CoV-2 test result without influenza testing does not exclude influenza.)
https://www.cdc.gov/flu/professionals/diagnosis/testing-guidance-for-clinicians.htm
Ironically, the information from both the WHO and the CDC is contradicted by the writers over at the Los Angeles County health department as it is stated quarantine and isolation are only required for “Covid-19” and that there are no significant differences in the treatment for both influenza and “Covid-19:”
What do I do if I am diagnosed with either virus? Are the treatment plans the same?
“When diagnosed with a positive for COVID-19, it is most important to quarantine and isolate to avoid spreading the virus to others. There is no other significant difference in treatment for COVID-19 and the flu. Complications for people at higher risk can be severe. Contact your doctor if you have had a fever for 3 or more days in a row.”
https://dhs.lacounty.gov/covid-19/testing/dual-covid-19-flue-testing-faq/
As we have the exact same symptoms of disease, the exact same inaccurate testing, and the exact same methods of treatment, it is pretty obvious that we are being given regurgitated plotlines and villains by the lazy inept writers of this show. If, however, one needs more convincing that this is the same actor just playing different parts, look no further than the slight of hand used to trick the masses in regards to the case counts:
As Covid-19 cases fall and masks come off, flu cases are rising
“Flu activity was declining from mid-December through January, according to the CDC. Around that time, Covid-19 cases were increasing. Then, as flu cases started to rise earlier this year, Covid-19 cases took a downturn.”
https://www.google.com/amp/s/amp.cnn.com/cnn/2022/03/25/health/flu-cases-rise-in-the-us/index.html
When “Covid” rises, the flu falls. When the flu rises, “Covid” falls. And vice versa. Around and around the cycle goes. This is how the hacks posing as creative visionaries trick the audience into believing that there are two separate “viruses” when in fact, all they do is skim off the case count of one to prop up the other. A recent example of this was seen in July 2022 in Mumbai:
As active Covid cases fall, influenza cases rise in city
“Drop in active cases is a good sign as it shows the disease load in the community is coming down. We will have to see in the coming days if cases continue to drop. With the latest genome sequencing reports, we know that BA.2 and BA.2.38- Omicron sub-variants have been the reason behind the surge in Mumbai/Maharashtra. Abroad too, we saw these variants led to a surge and within a few weeks, it saw a declining trend too. Here too, we are witnessing an early sign of decline in cases,” said Dr Pradip Awate, epidemiologist and state surveillance officer.
“Meanwhile, city doctors said they are also seeing a sudden spike in influenza cases. Dr Anil Ballani, general physician, Lilavati Hospital, Bandra, said, “We are seeing a spike in influenza cases. We are all worried about Covid-19, but not flu and the common cold. Covid cases now is mimicking influenza symptoms of high fever, cold, and throat pain. The only difference between the two is Covid is leading to weakness and persistent cough.”
The plot has become all too predictable. As the “Covid” cases drop, it will look as if the booster and counter measures are working to contain the “virus.” Meanwhile, the cases that were dropped as “Covid” conveniently become cases of the flu in order to increase urgency and to remind people to get their flu vaccine. This way, both diseases can coexist together and both vaccines can be utilized for the exact same symptoms of disease. All it takes is the use of inaccurate tests along with an increase or decrease in the amount of these tests being used to generate the fraudulent case numbers to make one appear to grow while the other subsides. This very scenario played out early on in the “pandemic” where flu testing was shunned in favor of “Covid-19” testing leading to a massive drop in cases and the disappearance of the flu. This can be seen by the CDC's own study where it was shown that, as the median number of samples sent for influenza testing dropped, so too did the positivity rate and the case count. Of course, “Covid” cases continued to rise. This was largely due to the preferential fraudulent testing and diagnosis of the same symptoms of disease being labelled as “Covid” over influenza:
Decreased Influenza Activity During the COVID-19 Pandemic — United States, Australia, Chile, and South Africa, 2020
“The median number of specimens tested for influenza each week decreased from 49,696 during September 29, 2019–February 29, 2020 (weeks 40–9), to 19,537 during March 1–May 16, 2020 (weeks 10–20), representing a 61% decrease. During these same two periods, influenza activity decreased 98%, from a median of 19.34% to 0.33% of submitted respiratory specimens testing positive for influenza.”
“Initially, declines in influenza virus activity were attributed to decreased testing, because persons with respiratory symptoms were often preferentially referred for SARS-CoV-2 assessment and testing.”
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7498167/
A March 2022 study from China also highlighted that there was a drastic decrease in influenza testing which resulted in a massive drop in cases:
Decreased Incidence of Influenza During the COVID-19 Pandemic
“More people were tested in 2019/2020 compared with the three other periods, while the smallest number was in 2020/2021 (P<0.01). But from February 2020, there was a sharp drop in the number of tests, from 25,070 in 2019/20 to 1107 in 2020/21 (Figure 1).”
“However, by the second half of the 2019/2020 flu season, only 8.56% and 8.56% (1089/12,729 and 1056/12,341) of the samples were sent for influenza A and B (Table 2). The number of samples tested increased by nearly 30% during the 2017/2018 and 2018/2019 seasons and the first half of the 2019/2020 season, but the number of samples tested dropped sharply in February-March 2019/2020 (P<0.01), coinciding with the start of COVID-19 (Figure 2).”
“In the present study, a sharp decrease in influenza tests and positivity was observed starting in February 2020, coinciding with the enforcement of sanitary measures in China. Only a small number of individuals were tested in 2020/2021, the specific reason for this may that people’s awareness of dense gatherings has increased due to the COVID-19 pandemic, reducing the spread of influenza to each other. But further research is needed.
Other papers also have showed similar results: Stamm et al showed that not only reduced respiratory syncytial virus cases, but also decreased influenza samples.13 The rate of influenza-positive tests also sharply decreased. Such a decrease was observed in other countries.14–16 Of course, there is a similar reduction trends founded in China.17”
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8932933/#!po=34.6154
Evidence from another 2022 study also backs up the conclusion that decreased testing for respiratory “viruses” other than “SARS-COV-2” resulted in the disappearance of influenza and other respiratory “viruses” during this pandemic:
Reduced spread of influenza and other respiratory viral infections during the COVID-19 pandemic in southern Puerto Rico
“Cases of influenza A began declining in the weeks leading up to March 15, 2020, suggesting that, at least with respect to influenza A, changes in testing or individual’s social distancing behavior taken ahead of the island-wide measures may have had an early impact on the number of influenza cases reported and are similar to decreases observed in the US [3, 20].”
“Our analysis had some limitations. Dramatic decreases in the number of tests samples were observed in our surveillance system, a situation observed across the region [11]. This could be due to a decrease in primary case detection during the period of mitigation measures and later or a decrease in testing for non-SARS-CoV-2 data.”
https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0266095
It is clear that the writers figured that they had a clever little trick to fool the audiences into believing that they had been introduced to a novel villain when it was nothing but a sleight of hand covering up the fact that the same actor was playing two roles. As the “new virus” appeared, the old one was hidden in the shadows by way of decreased appearances. All they had to do was write out the old respiratory “viruses” through decreased testing and prop up the novel “coronavirus” by way of shining the spotlight on it through preferential testing and more screentime. Thus, a “new” old villain emerged. However, after nearly three seasons of waning suspense, the novel villain has run its course. Now, it is time to reintroduce the old foe, setting the stage for an epic climactic showdown promising to reinvigorate the franchise. If the writers have their way, the same actor will be playing dual roles this winter in order to keep the masses frightened and entertained. However, if that plotline fails to win over audiences this winter, don't worry as the always-ahead-of-the-curve writers are already preparing for the future:
Based on the lack of original ideas and the vanishing viewership, it is time to pull the plug on this series.
Dr. Tom Cowan recently wrote an article asking virologists to answer 5 simple questions:
https://drtomcowan.com/blogs/blog/five-simple-questions-for-virologists
Attention-starved Jeremy Hammond thought he could refute Dr. Cowan's article based on the claims he made regarding purification and mock controls. While I do not want to link Hammond's inept article here (feel free to search for it if you feel like torturing yourself), I do want to highlight John Blaid's excellent response to Hammond:
https://johnblaid.substack.com/p/my-response-to-the-latest-article
Dr. Mark Bailey put together a masterful article rebutting the incorrect statements, illogical contradictions, and baseless accusations made against them by Dr. Roger Watson:
https://drsambailey.com/the-lazy-lies-of-roger-watson
Meanwhile, Dr. Sam Bailey had a truly engaging and fascinating discussion with researcher and author Jim West, possibly the first person to point out the Polio/DDT connection:
https://drsambailey.com/resources/videos/interviews/jim-west-the-toxicology-taboo/
Over at Humanley.com, Daniel Roytas had a












Hi Mike, wrote about your great post here on my newsletter:
https://protonmagic.substack.com/p/label-labeled-and-labeling-machines
Omg! thank you for putting this all in one place. My husband is a NP and articles like this help him stay straight, formulate his arguments with coworkers but more importantly, these articles remind him to forget testing and treat the patient.